CT Allows Nonsurgical Management of Some Lung Nodules
Released: June 23, 2015
At A Glance
- Nonsolid lung nodules can be safely monitored with annual low-dose CT which could help spare patients from unnecessary surgery and additional imaging.
- Nonsolid nodules could be due to inflammation, infection or fibrosis, but could also be cancerous or a precursor of cancer.
- Researchers analyzed results from 57,496 participants in the International Early Lung Cancer Program, a major worldwide initiative focused on reducing deaths from lung cancer.
- RSNA Media Relations
1-630-590-7762
media@rsna.org - Linda Brooks
1-630-590-7738
lbrooks@rsna.org - Emma Day
1-630-590-7791
eday@rsna.org
OAK BROOK, Ill. – People who have nonsolid lung nodules can be safely monitored with annual low-dose computed tomography (CT) screening, according to a new study published online in the journal Radiology. Researchers said the findings could help spare patients from unnecessary surgery and additional imaging.
Lung nodules are small masses of tissue in the lungs that can be benign or cancerous. They are classified as solid, part solid or nonsolid, based on their appearance on CT. In nonsolid lung nodules, normal lung tissue is visible through the nodule. Nonsolid nodules are visible on CT scans of the chest, and management of them is challenging.
"Nonsolid nodules could be due to inflammation, infection or fibrosis, but could also be cancerous or a precursor of cancer," said study co-author Claudia I. Henschke, Ph.D., M.D., from the Department of Radiology at Icahn School of Medicine at Mount Sinai in New York City. "For screening, we have to define which nodules need further workup and how quickly we have to do that workup."
In the new study, Dr. Henschke and colleagues analyzed results from 57,496 participants in the International Early Lung Cancer Program (I-ELCAP), a major worldwide initiative focused on reducing deaths from lung cancer. The patients underwent baseline and annual repeat screenings, and the researchers evaluated the prevalence of nonsolid nodules and their effect on long-term outcomes.
A nonsolid nodule was identified in 2,392 (4.2 percent) of the baseline screenings, and further analysis led to the diagnosis of 73 cases of cancer. A new nonsolid nodule was identified in 485 of 64,677 annual repeat screenings, or 0.7 percent, and 11 were diagnosed with Stage I cancer. Surgery was 100 percent curative in all cases, with a median follow-up since diagnosis of more than six years.
The nonsolid nodule developed a solid component—a warning sign of invasive cancer—in 22 cases prior to treatment. However, the median transition time from nonsolid to part-solid was more than two years. No cancers occurred in new nodules 15 millimeters or larger in diameter.
The findings suggest that nonsolid nodules of any size can be safely followed with low-dose CT at 12-month intervals to assess a potential transition to part-solid.
"The results show that if we see a nonsolid lung nodule of any size, we can tell people to come back in one year for another CT," Dr. Henschke said. "These findings are important for reducing unnecessary CT scans and possible biopsies or surgery in programs of CT screening for lung cancer."
One immediate benefit may be a reduction in the overtreatment of nodules, according to study co-author David F. Yankelevitz, M.D., from Mount Sinai.
"Many recommendations had been fairly aggressive with respect to nonsolid nodules," Dr. Yankelevitz said. "These results show that there is no reason to be aggressive in pursuit of cancer, so long as the nodules stay in this nonsolid form."
The study results also provide additional information to help in the shared decision-making process between physician and patient, Dr. Yankelevitz said. Patients can be assured that one-year low-dose CT screening intervals are sufficient, and also know that more aggressive treatment may be required if the nodules develop solid components.
"This is a major step forward for lung cancer screening protocols," Dr. Yankelevitz said. "It will help us cut down on the number of surgeries and unnecessary imaging tests."
"CT Screening for Lung Cancer: Nonsolid Nodules in Baseline and Annual Repeat Rounds." Collaborating with Drs. Henschke and Yankelevitz were Rowena Yip, M.P.H., James P. Smith, M.D., Mingzhu Liang, M.D., Ying Liu, M.D., Dong Ming Xu, M.D., Mary M. Salvatore, M.D., Andrea S. Wolf, M.D., and Raja M. Flores, M.D. As the Writing Committee for The International Early Lung Cancer Action Program Investigators Group.
Radiology is edited by Herbert Y. Kressel, M.D., Harvard Medical School, Boston, Mass., and owned and published by the Radiological Society of North America, Inc. (http://Radiology.RSNA.org)
RSNA is an association of more than 54,000 radiologists, radiation oncologists, medical physicists and related scientists promoting excellence in patient care and health care delivery through education, research and technologic innovation. The Society is based in Oak Brook, Ill. (RSNA.org)
For patient-friendly information on lung CT, visit RadiologyInfo.org.
Images (.JPG and .TIF format)
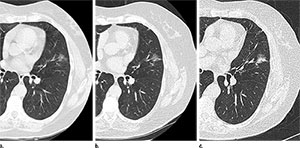
Figure 1. CT images in a 68-year-old smoker show (a) a nonsolid nodule (17 3 13 mm) in the left upper lobe at baseline screening, (b) the nodule remained nonsolid at follow-up 2 years later, and (c) a solid component emerged at follow-up 9 years later. At that time, it was resected, and the final diagnosis was 2.1-cm invasive adenocarcinoma.
High-res (TIF) version
(Right-click and Save As)
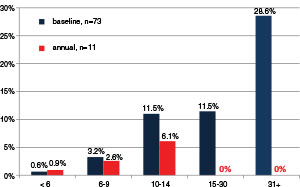
Figure 2. Graph shows the likelihood of diagnosing a lung cancer manifesting in a nonsolid nodule, sepa¬rately in the baseline (blue) and annual repeat (red) rounds of CT screening.
High-res (TIF) version
(Right-click and Save As)