Brain Injury Patterns Linked to Post-concussion Depression and Anxiety
Released: June 16, 2015
At A Glance
- Researchers using an MRI technique that measures the integrity of the brain’s white matter found unique white matter injury patterns in post-concussion patients who had depression or anxiety.
- Nearly 3.8 million people in the United States suffer concussions every year.
- The study also raises the possibility that some people diagnosed with non-traumatic depression may actually have experienced a subclinical traumatic event at some point earlier in their lives that may have contributed to the development of depression.
- RSNA Media Relations
1-630-590-7762
media@rsna.org - Linda Brooks
1-630-590-7738
lbrooks@rsna.org - Emma Day
1-630-590-7791
eday@rsna.org
OAK BROOK, Ill. – A new MRI study has found distinct injury patterns in the brains of people with concussion-related depression and anxiety, according to a new study published online in the journal Radiology. The findings may lead the way to improved treatment and understanding of these common disorders, researchers said.
Post-concussion psychiatric disorders like depression, anxiety and irritability can be extremely disabling for those among the nearly 3.8 million people in the United States who suffer concussions every year. The mechanisms underlying these changes after concussion—also known as mild traumatic brain injury—are not sufficiently understood, and conventional MRI results in most of these patients are normal.
For the new study, researchers from the University of Pittsburgh Medical Center (UPMC) in Pittsburgh used diffusion tensor imaging (DTI), an MRI technique that measures the integrity of white matter—the brain's signal-transmitting nerve fibers—to see if injuries to the nerves may be the root cause of these post-traumatic depression and anxiety symptoms.
The researchers obtained DTI and neurocognitive testing results for 45 post-concussion patients, including 38 with irritability, 32 with depression and 18 with anxiety, and compared the results with those of 29 post-concussion patients who had no neuropsychiatric symptoms.
"Using other concussion patients as our controls was a big advantage of our study," said lead author Lea M. Alhilali, M.D., assistant professor of radiology at UPMC. "When you are able to study a similar population with similar risk factors, you get much more reliable results."
The researchers saw unique white matter injury patterns in the patients who had depression or anxiety. Compared to controls, patients with depression had decreased fractional anisotropy (FA), a measure of the structural integrity of white matter connections, around an area near the deep gray matter of the brain that is strongly associated with the brain's reward circuit.
"The regions injured in concussion patients with depression were very similar to those of people with non-traumatic major depression disorder," Dr. Alhilali said. "This suggests there may be similar mechanisms to non-trauma and trauma-dependent depression that may help guide treatment."
Anxiety patients had diminished FA in a part of the brain called the vermis that helps modulate fear-related behaviors. Since the vermis has not been associated with dysfunction in non-traumatic anxiety disorders, this finding may indicate that different treatment targets are required for patients with anxiety after trauma, the researchers said.
No regions of significantly decreased FA were seen in patients with irritability relative to the control subjects.
"There are two major implications for this study," Dr. Alhilali said. "First, it gives us insight into how abnormalities in the brain occur after trauma, and second, it shows that treatments for non-trauma patients with neuropsychological symptoms may be applicable to some concussion patients."
The study also raises the possibility that some people diagnosed with non-traumatic depression may actually have experienced a subclinical traumatic event at some point earlier in their lives that may have contributed to the development of depression, she noted.
In the future, the researchers hope to compare DTI findings in concussion patients with depression to those of people who have non-trauma-related depressive disorders.
"Evaluation of White Matter Injury Patterns Underlying Neuropsychiatric Symptoms after Mild Traumatic Brain Injury." Collaborating with Dr. Ahlilali were Joseph A. Delic, M.D., Serter Gumus, M.D., and Saeed Fakhran, M.D.
Radiology is edited by Herbert Y. Kressel, M.D., Harvard Medical School, Boston, Mass., and owned and published by the Radiological Society of North America, Inc. (http://Radiology.RSNA.org)
RSNA is an association of more than 54,000 radiologists, radiation oncologists, medical physicists and related scientists promoting excellence in patient care and health care delivery through education, research and technologic innovation. The Society is based in Oak Brook, Ill. (RSNA.org)
For patient-friendly information on MRI of the brain, visit RadiologyInfo.org.
Images (.JPG and .TIF format)
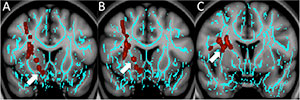
Figure 1. Coronal images derived from tract-based spatial statistics results and rendered on T1-weighted MR images from the Montreal Neurological Institute atlas show how patients with depression have significantly decreased fractional anisotropy in the region of A, the right nucleus accumbens (arrow) or “reward center,” as well as B, the anterior limb of the internal capsule (arrow) and C, the superior longitudinal fasciculus (arrow)—regions that are involved in depressive disorders in nontraumatic and traumatic settings.
High-res (TIF) version
(Right-click and Save As)
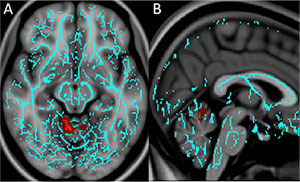
Figure 2. A, Axial and B, sagittal images derived from tract-based spatial statistics (TBSS) results and ren¬dered on T1-weighted MR images from the Montreal Neurological Institute atlas indicate that significant white matter differences in patients with mTBI and anxiety involve the cerebellar vermis, the region responsible for fear conditioning. Voxels with significant differences detected with TBSS were thickened by using the TBSS fill function into local tracts (red) and overlaid on the white matter skeleton (blue).
High-res (TIF) version
(Right-click and Save As)
