First Clinical Photon-Counting CT System Outperforms Current CT
Released: December 14, 2021
At A Glance
- The first photon-counting-detector (PCD) CT scanner available for clinical use outperforms current state-of-the art CT.
- PCD-CT systems have shown several advantages over standard CT, including suppression of electronic noise, improved spatial resolution, and reduced radiation dose.
- PCDs directly convert X-rays to electrical signal, facilitating small detector pixel designs without loss of dose efficiency.
- RSNA Media Relations
1-630-590-7762
media@rsna.org - Linda Brooks
1-630-590-7738
lbrooks@rsna.org - Imani Harris
1-630-481-1009
iharris@rsna.org
OAK BROOK, Ill. (December 14, 2021) — The first clinical photon-counting-detector (PCD) CT system available for patient care outperforms current state-of-the-art CT systems, according to a new study published in the journal Radiology.
PCD-CT systems have shown several advantages over standard CT, including suppression of electronic noise, improved spatial resolution, and reduced radiation dose. PCDs directly convert x-rays to electrical signal, facilitating small detector pixel designs without loss of geometric dose efficiency and allowing simultaneous multi-energy CT through the use of multiple energy thresholds.
Advances in the detector technology have facilitated translation of PCDs to human imaging at clinical doses and dose rates, demonstrating potential clinical benefits for patients.
With the introduction of the first clinical PCD-CT, the beneficial characteristics of PCDs can be realized in clinical practice. However, a comprehensive performance assessment is needed to confirm current clinical requirements are met and to provide performance benchmarks. Cynthia McCollough, Ph.D., and colleagues from the Department of Radiology at the Mayo Clinic in Rochester, Minnesota—working with representatives from Siemens Healthineers in Forchheim, Germany, and Siemens Medical Solutions in Malvern, Pennsylvania—set out to assess the technical performance of a clinical PCD-CT.
“PCD-CT is so exciting because it provides information that existing CT detectors – the types that we’ve used for over 50 years – previously just couldn’t capture,” said Dr. McCollough, director of Mayo Clinic’s CT Clinical Innovation Center. “It allows us to scan faster, with lower radiation and contrast media doses, while obtaining higher quality images with greater spatial detail and lower noise levels. For many clinical applications, the improvements in image quality are really striking.”
For the study, the researchers analyzed the technical performance of a dual-source PCD-CT system for standard and high-resolution collimations. Noise power spectrum, modulation transfer function, section sensitivity profile, iodine CT number accuracy in virtual monoenergetic images, and iodine concentration accuracy were measured.
Four participants were enrolled between May 2021 and August 2021 in this prospective study and scanned using similar or lower radiation doses compared to same-day exams performed using energy-integrating-detector (EID) CT. Four clinical indications (CT angiography of the coronary arteries and abdomen/pelvis, whole-body low-dose CT for skeletal surveillance, and temporal bone imaging) were selected to illustrate in humans the effects of PCD-CT’s improved technical performance in phantoms. PCD-CT scans were performed at the same or lower radiation dose relative to the clinical exam.
The results showed that PCD-CT demonstrated superior spatial resolution relative to current CT systems and improved noise properties and multi-energy temporal resolution relative to similarly configured EID-CT.
The high-resolution mode of the PCD-CT demonstrated 125-micron in-plane spatial resolution and 0.3 mm longitudinal resolution, the smallest reported to date for a clinical CT system. The PCD-CT system provided 66-ms temporal resolution multi-energy imaging in dual source mode. Noise reduction (up to 47%) or dose reduction (up to 30%) were achieved in study participants using the PCD-CT system relative to a similar CT system equipped with conventional detectors.
“Every time that CT technology has advanced to provide new technical capabilities, new clinical applications have followed,” Dr. McCollough said. “With PCD-CT, we are seeing anatomy and disease at a resolution that has never before been achieved in patients, and that is providing physicians new information and insights—insights that can change patient management. In patients with coronary artery disease, for example, PCD-CT can provide diagnostic quality images in patients who previously were not good candidates for CT imaging of their coronary arteries. This will spare many patients from having to have more invasive types of testing.”
“First Clinical Photon-counting Detector CT System: Technical Evaluation.” Collaborating with Dr. McCollough was Kishore Rajendran, Ph.D., Martin Petersilka, Ph.D., André Henning, Ph.D., Elisabeth R. Shanblatt, Ph.D., Bernhard Schmidt, Ph.D., Thomas G. Flohr, Ph.D., Andrea Ferrero, Ph.D., Francis Baffour, M.D., Felix E. Diehn, M.D., Lifeng Yu, Ph.D., Prabhakar Rajiah, M.D., Joel G. Fletcher, M.D., and Shuai Leng, Ph.D.
This study was supported by the National Institutes of Health under award numbers R01 EB028590 and supported in kind by Siemens Healthineers GmbH, who own the evaluated system under the terms of a sponsored research agreement with the Mayo Clinic. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institute of Health. The device described is CE labeled and has received 510k clearance by the U.S. Food and Drug Administration.
Radiology is edited by David A. Bluemke, M.D., Ph.D., University of Wisconsin School of Medicine and Public Health, Madison, Wisconsin, and owned and published by the Radiological Society of North America, Inc. (https://pubs.rsna.org/journal/radiology)
RSNA is an association of radiologists, radiation oncologists, medical physicists and related scientists promoting excellence in patient care and health care delivery through education, research and technologic innovation. The Society is based in Oak Brook, Illinois. (RSNA.org)
For patient-friendly information on CT, visit RadiologyInfo.org.
Images (JPG, TIF):
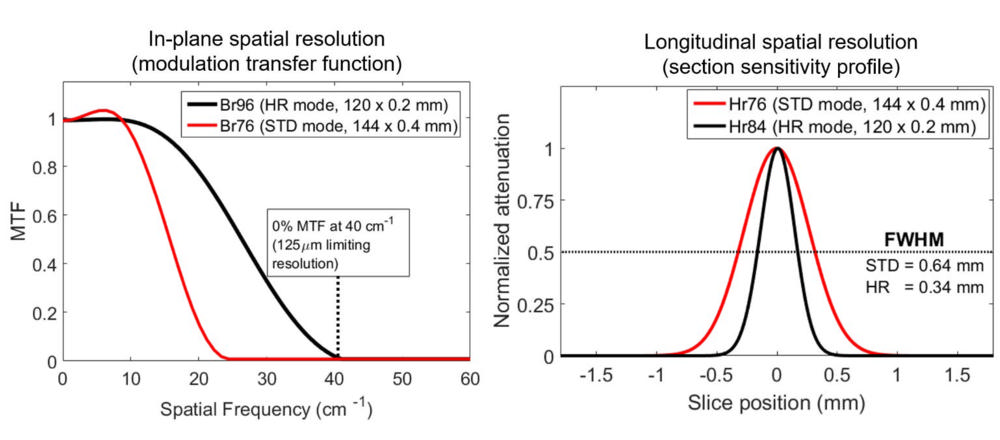
Figure 1. Modulation transfer functions (left) and section sensitivity profiles (right) for the standard (STD) and high-resolution (HR) collimations of the photon-counting-detector CT system. A limiting in-plane spatial resolution of 125 microns (µm) and a full-width-half-maximum (FWHM) value of 0.34 mm (section sensitivity profile) were achieved using the HR collimation. Br: Body regular reconstruction kernel, Hr: Head regular reconstruction kernel, MTF: Modulation transfer function.
High-res (TIF) version
(Right-click and Save As)
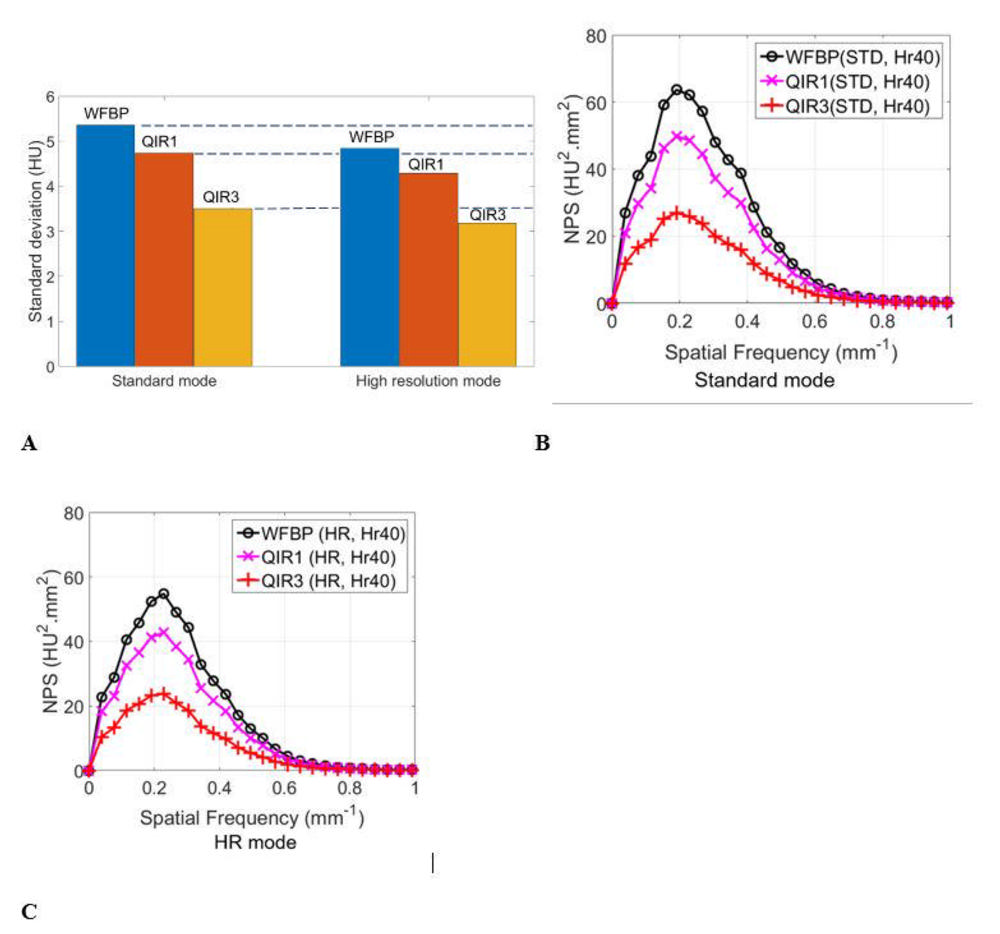
Figure 2. Image noise was reduced by 11.5% and 34.5% for quantum iterative reconstruction (QIR) images using strengths 1 and 3, respectively (labelled QIR1 and QIR3), relative to weighted-filtered-back-projection (WFBP) using a Head-regular-40 (Hr40) kernel as shown in A. Horizontal dotted lines assist the reader in comparing noise levels between the collimation settings. Noise power spectra (NPS) for standard (STD) (B) and high resolution (HR) (C) collimations demonstrate QIR reduced the noise magnitude (height of the curve) compared to WFBP images for both collimations and strengths without shifting the spatial frequency of the peak of the noise power spectrum (NPS) curves, indicating that only the amount of noise, and not the noise texture, is impacted with use of QIR.
High-res (TIF) version
(Right-click and Save As)
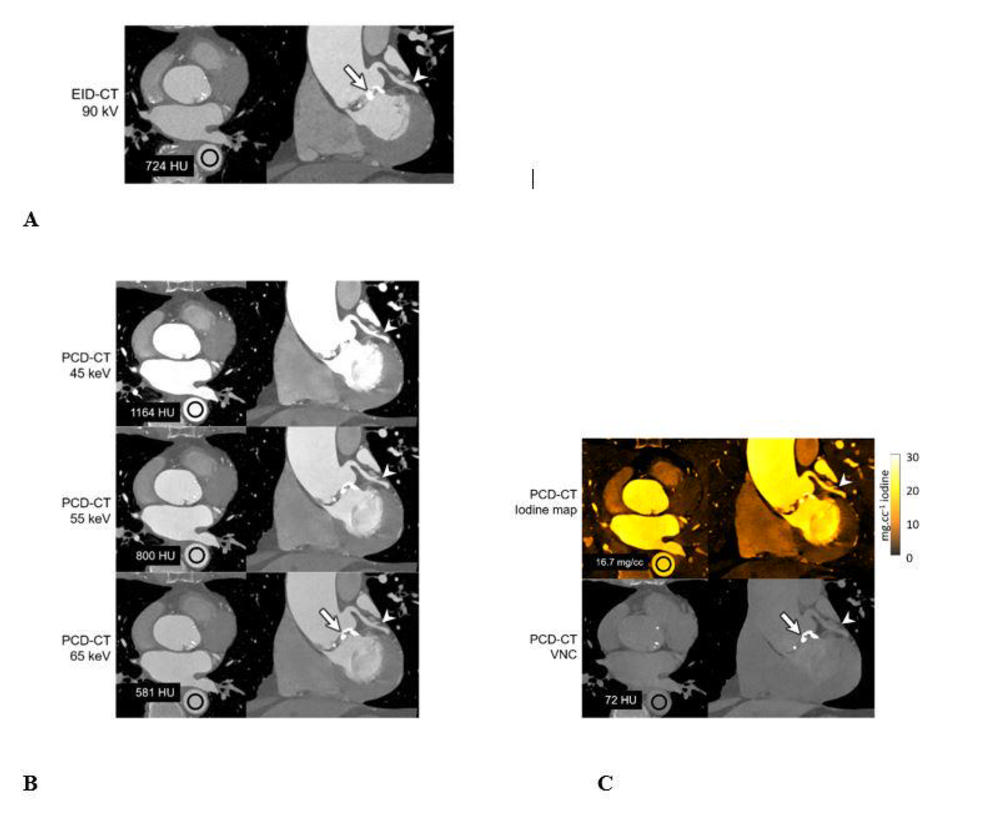
Figure 3. A 71-year-old male scanned on energy-integrating-detector (EID)-CT (A) and photon-counting-detector (PCD)-CT (B, C) with dual-source geometry to achieve 66-ms temporal resolution. Axial CT images are shown in the left column and oblique coronal images are shown in the right column. While the EID-CT exam is limited to single energy data (A) at this temporal resolution, the multi-energy capabilities of the PCD-CT system allowed creation of low energy (45, 55 keV) virtual mono-energetic images (VMIs) (B), which showed increased iodine signal (shown as mean HU measurements in region-of-interests) compared to EID-CT despite an 18% decrease (A: 110 mL versus B/C: 90 mL iohexol) in administered contrast volume (mean CT numbers for the regions of interest shown in black are given in the left column of images). The use of VMIs adds to the inherently higher iodine contrast-to-noise ratio possible with PCD-CT and provided clearer delineation of a branch of the left coronary artery (white arrowheads, right column). Increasing the VMI energy (65 keV or higher) decreased calcium blooming relative to EID-CT (white arrow, right column, A and B). Absolute iodine concentration was measured using the iodine map images (mean concentration in mg/cc unit shown in region-of-interest) and the virtual-non-contrast images used to visualize calcifications having similar attenuation to the iodinated blood (white arrow, right column, C). Reconstruction kernels used: Body-vascular (Bv) 40 (EID-CT 90-kV, A), Bv48 (PCD-CT VMIs, B), Quantitative-regular (Qr) 40 (PCD-CT iodine map and VNC, C). Display window/level: 2000/200 HU for EID-CT and PCD-CT VMIs, 30/15 mg.cc-1 for iodine map and 1000/100 HU for VNC image.
High-res (TIF) version
(Right-click and Save As)
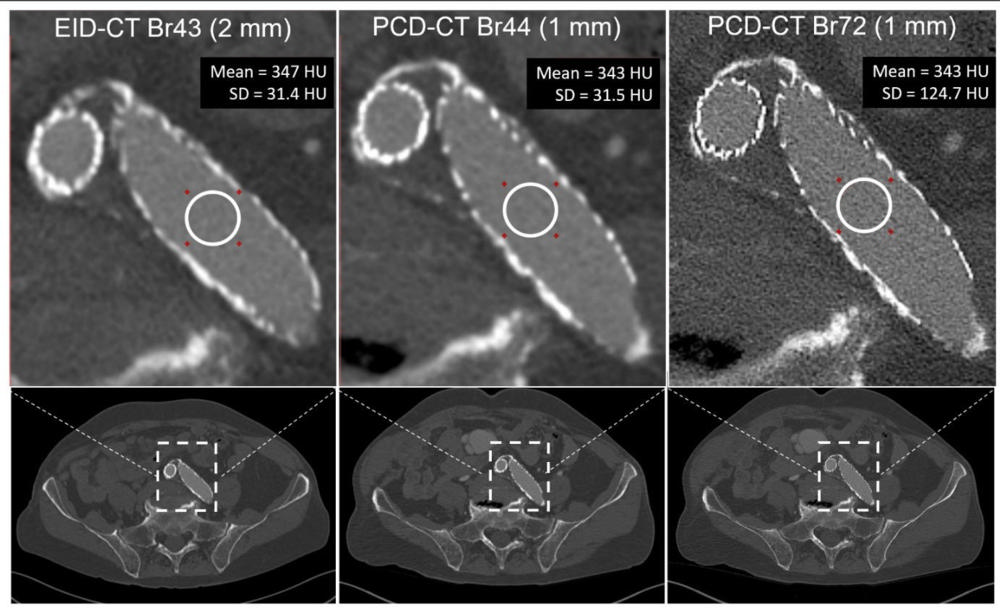
Figure 4. An 85-year-old male with aortobiiliac stent graft scanned for angiographic examination on energy-integrating-detector CT (EID-CT) at 100 kV (axial CT image, left column) and high-resolution photon-counting-detector (PCD) CT (axial T3D image, includes photon energies from 20 to 120 keV) (center and right columns). Both scans used the same radiation dose (10 mGy). The top row images correspond to an enlarged view of the rectangular region of interest displayed in the bottom row. The PCD-CT image in the right column was created using a sharper resolution (body-regular 72 kernel) than is possible to achieve on EID-CT to reduce stent blooming and improve delineation of the struts at the expense of increased image noise (shown as standard deviation, SD measurements in region-of-interests). Display window/level = 1800/440 HU.
High-res (TIF) version
(Right-click and Save As)
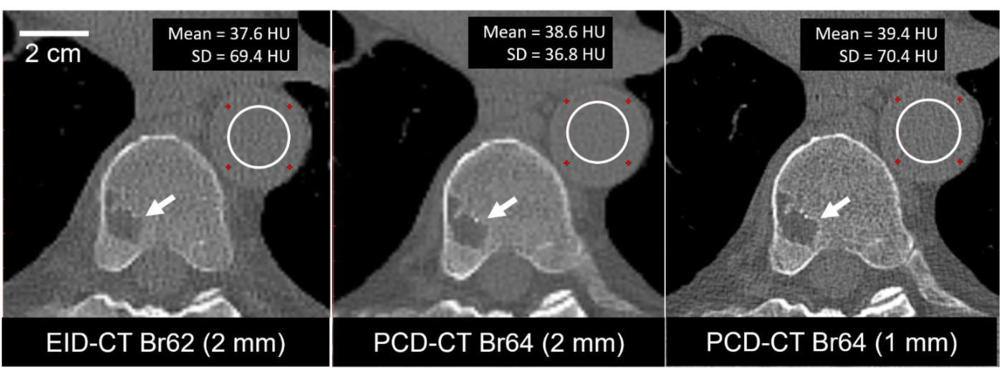
Figure 5. A 74-year-old male clinically indicated for a whole-body low-dose CT skeletal survey for multiple myeloma. Energy-integrating-detector CT (EID-CT) scan (axial image, left) and high-resolution photon-counting-detector CT (PCD-CT) scan (axial image, center and right) were acquired using the same radiation dose (4.2 mGy). PCD-CT images (center) using the same section thickness (2 mm) as EID-CT images (left) showed 47% lower noise (69.4 HU vs. 36.8 HU). Use of thinner (1 mm) section thickness (right) and 1024×1024 matrix resulted in image noise comparable to EID-CT and improved the delineation of a vertebral lesion (arrow). Display window/level = 1500/150 HU. SD: standard deviation of pixel values in the region-of-interest.
High-res (TIF) version
(Right-click and Save As)

Figure 6. A 72-year-old male scanned on energy-integrating detector (EID) CT and photon-counting detector (PCD) CT for temporal bone examination. Right temporal bone images (oblique axial plane) from EID-CT were reconstructed using ultra-high-resolution-regular (Ur) kernels - Ur77 and Ur85 at 0.4-mm section thickness and PCD-CT using head-regular (Hr) kernels - Hr76 and Hr84 at 0.2-mm section thickness. PCD-CT show better trabecular detail and delineation of the stapes compared to EID-CT (images A/B versus C/D), despite use of 30% (46.4 versus 32.6 mGy) lower dose for PCD-CT. Display window/level = 3800/700 HU. SD: standard deviation of pixel values in the region-of-interest.
High-res (TIF) version
(Right-click and Save As)
