Digital Mammography Increases Breast Cancer Detection
Released: December 11, 2018
At A Glance
- Digital mammography increased cancer detection by an overall rate of 14 percent in a large UK study.
- Data from 80 facilities and 11.3 million screening exams in the English National Health Service Breast Cancer Screening Program were analyzed.
- In first screening mammograms for women between the ages of 45 and 52, digital mammography increased the overall cancer detection rate by 19 percent with no increase in recall rates.
- RSNA Media Relations
1-630-590-7762
media@rsna.org - Linda Brooks
1-630-590-7738
lbrooks@rsna.org - Dionna Arnold
1-630-590-7791
darnold@rsna.org
OAK BROOK, Ill. — The shift from film to digital mammography increased the detection of breast cancer by 14 percent overall in the United Kingdom without increasing the recall rate, according to a major new study appearing in the journal Radiology.
Digital mammography was introduced into clinical use more than 15 years ago and has been widely adopted due to the numerous advantages it has over its predecessor, screen film mammography.
"Image quality with digital mammography is improved over that of screen film mammography," said radiologist and study coauthor Rosalind M. Given-Wilson, M.B.B.S., from St. Georges University Hospitals NHS Foundation Trust in London. "In particular, digital mammography provides the ability to visualize calcifications and see through denser tissue, and it allows the reader to adjust the image."
Dr. Given-Wilson and colleagues assessed digital mammography's impact on cancer detection using data from the 80 facilities of the English National Health Service Breast Cancer Screening Program. The huge trove of data combined with estimates of digital mammography usage enabled the researchers to measure the effect of digital mammography in 11.3 million screening exams in women between the ages of 45 and 70.
The overall cancer detection rate was 14 percent greater with digital mammography, with substantially higher detection of grade 1 and grade 2 invasive cancers—early-stage cancers that could advance to life-threatening disease if not detected and treated early enough.
At first screening exams for women aged 45 to 52, digital mammography increased the overall detection rate by 19 percent. Importantly, the higher sensitivity of digital mammography did not increase the recall rate—the rate at which women are called back for additional screening based on suspicious results.
"This improvement happened in the absence of other changes in the English screening program, such as a change in recall rate or introduction of computer-aided detection, so we can be clear that the increased rate of detection is due to the change in technology," Dr. Given-Wilson said.
Digital mammography increased the detection of some types of cancers more than others. For instance, digital mammography significantly increased the detection of ductal carcinoma in situ, or DCIS, an early-stage cancer confined to the milk ducts of the breast, at both first screens and subsequent screens.
"These results confirm that digital mammography is superior to screen film mammography in finding invasive cancers and DCIS," Dr. Given-Wilson said. "Women are more likely to have a cancer detected with a digital mammogram."
While digital mammography improved detection of grade 1 and 2 cancers, the researchers found no improvement in the detection of grade 3 invasive cancers. Grade 3 cancers are faster-growing and more likely to spread than grade 1 and 2 cancers.
The researchers are looking at the radiological features of grade 3 cancers on digital mammography to see if optimizing the image for these lesions, which are often nonspecific and ill-defined soft tissue densities, can aid detection. They are also studying the relationship between grade 3 cancers and subsequent interval cancers, or cancers that appear between screenings.
"Impact of Digital Mammography on Cancer Detection and Recall Rates: 11.3 Million Screening Episodes in the English National Health Service Breast Cancer Screening Program." Collaborating with Dr. Given-Wilson were Roger G. Blanks, Ph.D., Matthew G. Wallis, FRCR, Rupert Alison, M.Sc., Olive Kearins, M.Sc., Jacquie Jenkins, M.P.H., and Julietta Patnick, B.A.
Radiology is edited by David A. Bluemke, M.D., Ph.D., University of Wisconsin School of Medicine and Public Health, Madison, Wis., and owned and published by the Radiological Society of North America, Inc. (http://radiology.rsna.org/)
RSNA is an association of over 54,000 radiologists, radiation oncologists, medical physicists and related scientists, promoting excellence in patient care and health care delivery through education, research and technologic innovation. The Society is based in Oak Brook, Ill. (RSNA.org)
For patient-friendly information on mammography, visit RadiologyInfo.org.
Images (.JPG and .TIF format)
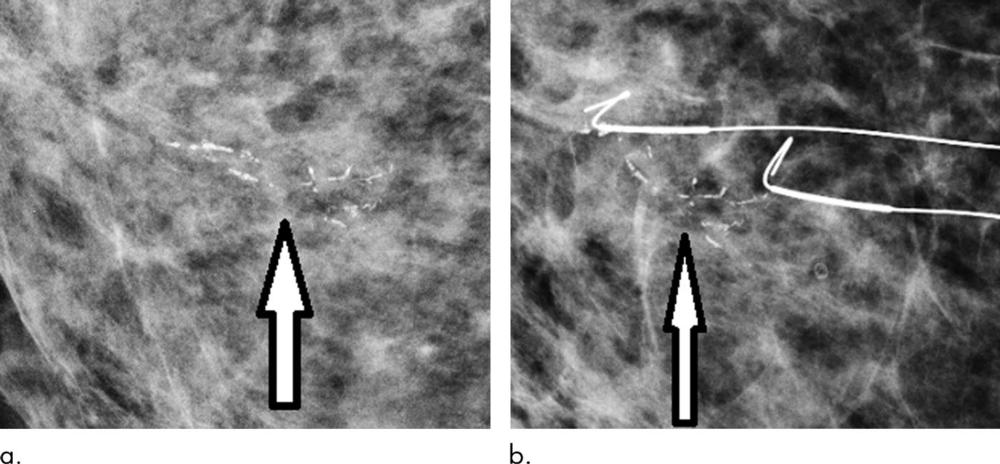
Figure 1. Routine screening mammograms from a 73-year-old woman show (a) 25-mm new casting calcifications representing ductal carcinoma in situ (DCIS) (arrow) in medial right breast. (b) Patient was treated with surgical excision guided by bracketed wires. Histologic examination showed high-nuclear-grade DCIS.
High-res (TIF) version
(Right-click and Save As)
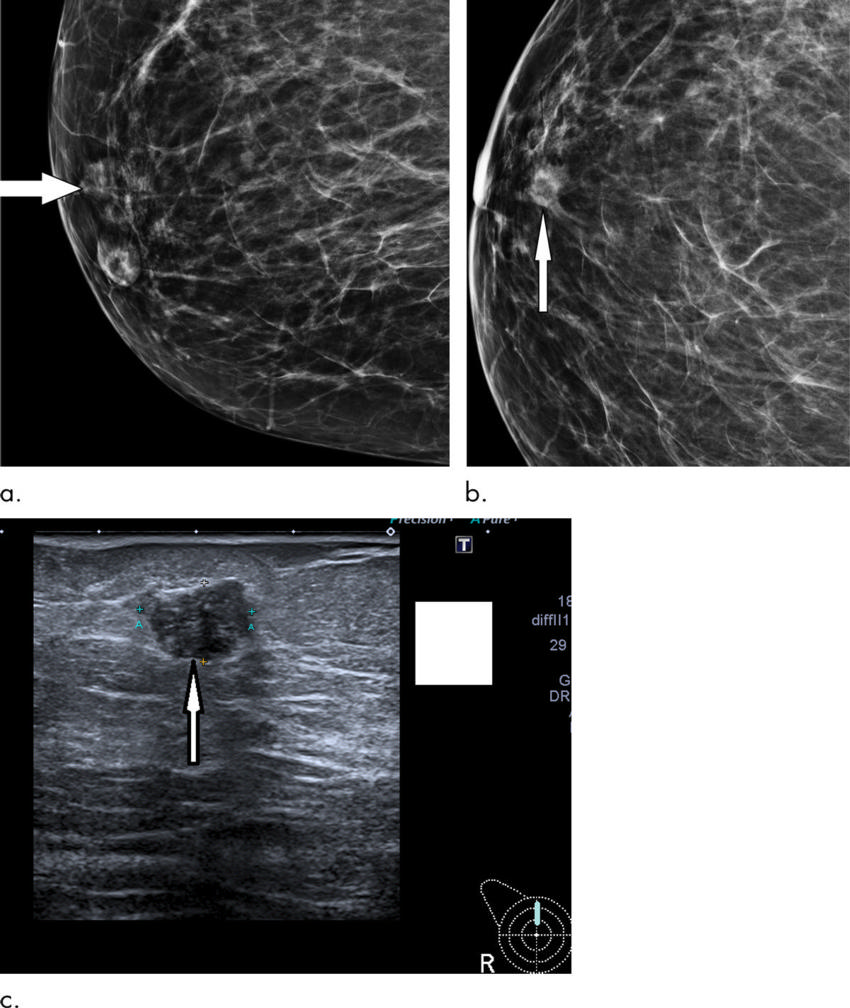
Figure 2. Routine screening mammogram in a 67-year-old woman shows subtle 12-mm asymmetric density with ill-defined margins representing small grade 3 cancer (arrow) on (a) lateral oblique view and (b) cranio-caudal view; it is difficult to see even on digital mammogram in a nondense breast. Subsequent clinical examination was normal. (c) US confirmed 12-mm irregular hypoechoic mass (arrow). Patient underwent wire-guided surgical excision and sentinel node biopsy. Final histologic examination showed 14-mm grade 3 invasive ductal carcinoma, which was node negative.
High-res (TIF) version
(Right-click and Save As)
