Stent Retrievers Improve Odds for Ischemic Stroke Patients
Released: April 19, 2016
At A Glance
- Timely endovascular treatment to restore blood flow to the brain significantly improves functional outcomes in patients with acute ischemic stroke.
- Restoration of blood flow within 2.5 hours of symptom onset was associated with minimal or no disability in 91 percent of patients.
- Patients who were transported to a stroke center instead of an endovascular-capable center experienced a treatment delay of nearly 2 hours.
- RSNA Media Relations
1-630-590-7762
media@rsna.org - Linda Brooks
1-630-590-7738
lbrooks@rsna.org
OAK BROOK, Ill. — Timely treatment with endovascular therapy to restore blood flow to the brain significantly improves functional outcomes in patients with acute ischemic stroke, according to a new study published online in the journal Radiology. The findings underscore the importance of getting stroke patients to the correct level of care quickly and efficiently, researchers said.
"The earlier that patients with acute ischemic stroke get to a hospital offering the appropriate treatment, the higher the likelihood is of a good outcome," said the study's lead author, Mayank Goyal, M.D., FRCPC, from the University of Calgary in Calgary, Alberta.
Acute ischemic stroke, or a stroke caused by blockages in arteries carrying blood to the brain, accounts for almost 90 percent of all strokes. Brain tissue deprived of oxygen-bearing blood can die quickly, resulting in long-term functional impairments for the patient such as difficulty walking or speaking.
In recent years, important advances have been made in stroke care, including intravenous tissue plasminogen activator (IV t-PA) and stent retrievers. IV t-PA is a protein that breaks down blood clots. Stent retrievers are mesh devices that are threaded through a blood vessel in the groin to blocked arteries in the head under X-ray guidance to grab and remove the clot.
In the new study, researchers analyzed data on patients treated with both IV t-PA and stent retrievers from the Solitaire With the Intention For Thrombectomy as PRIMary Endovascular Treatment (SWIFT PRIME) Trial to learn more about the clinical relevance of the duration of time from symptom onset to clot removal.
Results underscored the importance of timely clot removal. Restoration of blood flow to the brain within 2.5 hours of symptom onset was associated with functional independence, or minimal or no disability, in 91 percent of patients. The likelihood of functional independence was 10 percent higher in patients treated within 2.5 hours compared to patients treated between 2.5 and 3.5 hours after stroke onset. Every 60-minute delay after 3.5 hours resulted in a 20 percent lower likelihood of functional independence.
However, not all facilities are trained or equipped to offer these treatments in the crucial first hours after a stroke.
The researchers found that inter-facility transfer times represented a significant source of delay in the management of the patients. Time from onset of symptoms to the initiation of clot removal averaged more than 4.5 hours for patients who initially arrived to a referring facility, compared with only 3 hours for patients who presented directly to an endovascular-capable center with stent- retriever services available.
"Two-thirds of the patients in our study went directly to the endovascular-capable center and one-third went to a primary stroke center," Dr. Goyal said. "For those who went to the stroke center, there was a loss of about two hours in overall workflow, which is pretty significant."
The study results highlight the importance of tracking endovascular workflow times and providing feedback to maintain good results in the acute management of stroke.
"Given the substantial decrease in functional independence with increase in time to restoration of blood flow, every step in the work up and treatment of these patients should be weighed against the time spent versus the potential benefit," Dr. Goyal said.
"Analysis of Workflow and Time to Treatment and Its Impact on Outcome in Endovascular Treatment of Acute Ischemic Stroke Outcome: Results from the SWIFT PRIME Randomized Controlled Trial." Collaborating with Dr. Goyal on behalf of the SWIFT PRIME investigators were Ashutosh P. Jadhav, M.D., Ph.D., Alain Bonafe, M.D., Hans Diener, M.D., Vitor Mendes Pereira, M.D., Elad Levy, M.D., Blaise Baxter, M.D., Tudor Jovin, M.D., Reza Jahan, M.D., Bijoy K. Menon, M.D., and Jeffrey L. Saver, M.D.
Radiology is edited by Herbert Y. Kressel, M.D., Harvard Medical School, Boston, Mass., and owned and published by the Radiological Society of North America, Inc. (http://radiology.rsna.org/)
RSNA is an association of more than 54,000 radiologists, radiation oncologists, medical physicists and related scientists, promoting excellence in patient care and health care delivery through education, research and technologic innovation. The Society is based in Oak Brook, Ill. (RSNA.org)
For patient-friendly information on stroke, visit RadiologyInfo.org.
Images (.JPG and .TIF format)
and Video clips (.mp4 format)
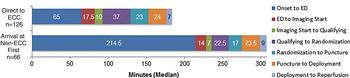
Figure 1. Graph of time intervals in patients treated within the same institution—an endovascular-capable center (ECC)—versus those who were transferred from another facility after receiving intravenous tPA therapy. Deployment = device deployment, puncture = groin puncture, qualifying = qualifying image acquisition.
High-res (TIF) version
(Right-click and Save As)
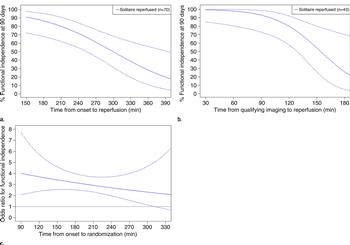
Figure 2. Graphs show (a) rates of functional independence in relation to symptom onset to reperfusion time in all patients in the endovascular arm, (b) rates of functional independence in relation to qualifying imaging acquisition to reperfusion time in ECC patients only, and (c) the odds ratio for functional independence of patients in the endovascular arm versus the tPA-only arm in relation to symptom onset to randomization time. The solid line represents the point estimate of the odds ratio across time, while the dotted lines collectively represent the 95 percent CI (upper and lower values) for the odds ratio.
High-res (TIF) version
(Right-click and Save As)
