Smoking Impedes Embolization Treatment in Lungs
Released: July 30, 2019
At A Glance
- Smoking reduced the chance of a successful procedure to treat blood vessel abnormalities in the lungs.
- Researchers looked at 103 patients who underwent embolization for pulmonary arteriovenous malformations.
- Smokers had a five-year PAVM persistence rate of 26.3 percent compared with 13.5 percent in nonsmokers.
- RSNA Media Relations
1-630-590-7762
media@rsna.org - Linda Brooks
1-630-590-7738
lbrooks@rsna.org - Dionna Arnold
1-630-590-7791
darnold@rsna.org
OAK BROOK, Ill. — Smoking reduces the chances of a successful procedure to treat blood vessel abnormalities in the lungs, according to a study published in the journal Radiology.
Pulmonary arteriovenous malformations (PAVMs) are abnormal connections between arteries and veins in the lungs. The abnormalities can become symptomatic and lead to potentially dangerous complications. PAVMs are strongly associated with an inherited disorder called Hereditary Hemorrhagic Telangiectasia (HHT).
"HHT is a disease that can manifest with patients having AVMs in their lungs," said study senior author Sanjay Misra, M.D., an interventional radiologist at the Mayo Clinic Department of Radiology in Rochester, Minn. "When these AVMs become symptomatic, we are asked to embolize them using coils."
In the embolization procedure, a catheter is threaded from a large blood vessel in the leg to the site of the PAVM. A small coil is then inserted to block the PAVM. The procedure is highly effective, but the PAVMs will persist in some patients.
For the new study, Dr. Misra and colleagues wanted to see how smoking might affect post-embolization PAVM persistence rates. They looked at 103 patients with HHT who underwent embolization for a total of 373 PAVMs. The patients were classified into smoking or non-smoking groups.
Smokers faced a higher rate of PAVM persistence following treatment than those who had never smoked. Patients reporting active tobacco use at the time of PAVM embolization had a five-year persistence rate of 26.3 percent compared with 13.5 percent in inactive smokers.
PAVMs persisted after treatment in more than a third of smokers with more than 20 pack-years, compared with only 12.2 percent of nonsmokers. Pack years is a measure of smoking intensity that accounts for how long and how much a person has smoked.
"Our five-year data showed that the cumulative incidence of persistence was 17.3 percent, or almost one in five patients," Dr. Misra said. "Smoking more than 20 pack years was associated with a fivefold increase in PAVM recurrence."
While the study did not assess the reason for the post-embolization persistence of PAVMs in smokers, previous research has linked smoking with inflammation and abnormalities in the formation of new blood vessels.
"Smoking creates an inflammatory response," Dr. Misra said. "More inflammation creates a greater likelihood of failure for smokers compared to those who never smoked."
The findings, if confirmed in larger studies, could be used to advise patients with HHT who might be considering embolization for PAVMs.
"Smoking cessation is very important if these patients want to help themselves and avoid further procedures," Dr. Misra said. "We should urge current smokers to stop smoking before treatment."
"Smoking Significantly Impacts Persistence Rates in Embolized Pulmonary Arteriovenous Malformations in Patients with Hereditary Hemorrhagic Telangiectasia." Collaborating with Dr. Misra were Mustafa M. Haddad, M.D., Emily C. Bendel, M.D., William S. Harmsen, M.S., and Vivek N. Iyer, M.D.
Radiology is edited by David A. Bluemke, M.D., Ph.D., University of Wisconsin School of Medicine and Public Health, Madison, Wis., and owned and published by the Radiological Society of North America, Inc. (https://pubs.rsna.org/journal/radiology)
RSNA is an association of over 53,400 radiologists, radiation oncologists, medical physicists and related scientists, promoting excellence in patient care and health care delivery through education, research and technologic innovation. The Society is based in Oak Brook, Ill. (RSNA.org)
For patient-friendly information on embolization, visit RadiologyInfo.org.
Images (.JPG and .TIF format)

Figure 1. Inclusion flowchart. HHT = hereditary hemorrhagic telangiectasia, PAVM = pulmonary arteriovenous malformation.
High-res (TIF) version
(Right-click and Save As)

Figure 2. Images in a 52-year-old woman with hereditary hemorrhagic telangiectasia demonstrating on left pulmonary artery angiogram an arteriovenous malformation (AVM) at, A, B, the left base. C, Selective angiogram after embolization of the AVM by using coils. D, E, Angiogram shows embolization for persistence treated with repeat embolization performed 2 years after initial embolization.
High-res (TIF) version
(Right-click and Save As)

Figure 3. Images in a 68-year-old woman with hereditary hemorrhagic telangiectasia (HHT) and a smoking history of 40 pack-years demonstrating, A, a complex arteriovenous malformation (AVM) at the left base on intravenous contrast-enhanced chest CT scan. B, C, Left pulmonary artery angiogram shows the AVM. D, Image after embolization and after placement of an Amplatzer plug. E, A selective angiogram of the second arterial blood supply to the AVM. F, Angiogram after coil embolization. (Fig 3 continues).
High-res (TIF) version
(Right-click and Save As)
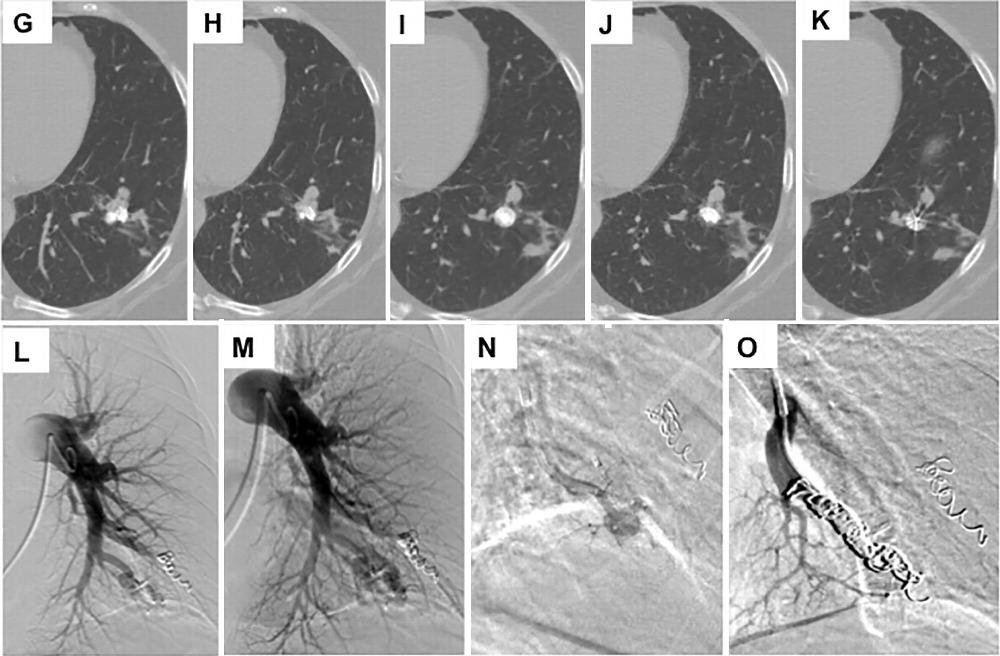
Figure 3 (Continued). G–K, Selective 1.5-mm intravenous contrast-enhanced axial CT images show persistence of the AVM 1 year later. L–M, Left pulmonary artery angiogram shows persistence. N, Selective catherization of the artery supplying the AVM. O, Angiogram after embolization of the AVM after coil embolization.
High-res (TIF) version
(Right-click and Save As)