MRI Helps Predict Preterm Birth
Released: March 15, 2016
At A Glance
- Early dilation of the cervix during pregnancy can lead to premature delivery.
- Women with a short cervix and suspected fetal or placental abnormalities were examined with an MRI technique called diffusion-weighted imaging (DWI).
- Cell density measurements derived from DWI results predicted which patients were at greater risk for impending preterm delivery.
- RSNA Media Relations
1-630-590-7762
media@rsna.org - Linda Brooks
1-630-590-7738
lbrooks@rsna.org
OAK BROOK, Ill. — MRI of the cervix is more accurate than ultrasound at predicting if some women will have a preterm birth, according to a new study from Italy appearing in the online edition of Radiology.
Early dilation of the cervix, a neck of tissue connecting the uterus with the vagina, during pregnancy can lead to premature delivery. Women in their second trimester of pregnancy with a cervix measuring 15 millimeters or less, as seen on ultrasound, are considered to be at higher risk of preterm birth. However, ultrasound has limitations as a predictor of preterm birth, as it does not provide important information on changes in cervical tissue in the antepartum phase just before childbirth.
"A better understanding of the process of antepartum cervical remodeling, loosely divided in two distinct phases called softening and ripening, is critical to improve the diagnosis of cervical malfunction and anticipate the occurrence of birth," said the study's lead author, Gabriele Masselli, M.D., from the Radiology Department at Sapienza University in Rome.
To learn more, Dr. Masselli and colleagues used an MRI technique called diffusion-weighted imaging (DWI) to examine pregnant women who had been referred for suspected fetal or placental abnormality. DWI reveals differences in the mobility of water molecules in tissue and the results can be used to create apparent diffusion coefficient (ADC) maps that provide a measure of local cell density. DWI has been increasingly used for abdominal and pelvic diseases, but has not been tested for the evaluation of the uterine cervix in pregnant patients.
Each of the 30 pregnant women in the study had a sonographically short cervix and a positive fetal fibronectin test between 23 and 28 weeks of gestation. Fetal fibronectin is a glue-like protein that helps hold the fetal sac to the uterine lining, and the presence of it before week 35 of gestation may indicate a higher risk of preterm birth.
Of the 30 women, eight, or 27 percent, delivered within a week of the MRI examination. The other 22 delivered an average of 55 days later. The researchers compared differences in ADC values at MRI between two areas of the cervix: the inner, subglandular zone and the outer, stromal area. While stromal ADC and sonographic cervical length showed no difference between both groups, the subglandular ADC was higher in patients with impending delivery, suggesting an increased mobility of water molecules in that area consistent with cervical ripening.
"Our results indicate that a high ADC value recorded at the level of the subglandular area of the cervix is associated with the imminent delivery of asymptomatic patients with a short cervix," Dr. Masselli said. "In detail, the subglandular ADC was inversely correlated to the time interval between MRI and delivery and therefore emerged as a powerful imaging biomarker in evaluating patients with impending delivery."
The research team is planning larger, multicenter trials to confirm the role of subglandular ADC analysis in predicting preterm birth, Dr. Masselli said.
"Are Second Trimester Apparent Diffusion Coefficient Values of the Short Uterine Cervix Associated with Impending Preterm Delivery?" Collaborating with Dr. Masselli were Giuseppina Perrone, M.D., Karen Kinkel, M.D., Marco Di Tola, M.D., Francesca Laghi, M.D., Gianfranco Gualdi, M.D., and Roberto Brunelli, M.D.
Radiology is edited by Herbert Y. Kressel, M.D., Harvard Medical School, Boston, Mass., and owned and published by the Radiological Society of North America, Inc. (http://radiology.rsna.org/)
RSNA is an association of more than 54,000 radiologists, radiation oncologists, medical physicists and related scientists, promoting excellence in patient care and health care delivery through education, research and technologic innovation. The Society is based in Oak Brook, Ill. (RSNA.org)
For patient-friendly information on MRI during pregnancy, visit RadiologyInfo.org.
Images (.JPG and .TIF format)
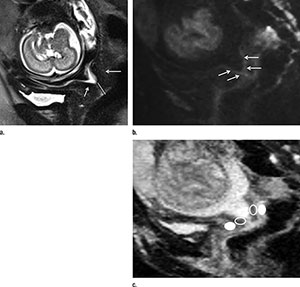
Figure 1. Images in a 29-year-old woman at 28 weeks of gestation with a sonographic cervical length of 6 mm who was referred for evaluation of suspected corpus callosum dysgenesis. (a) MR image shows a short cervix (white line) with funneling. The cervical canal appears as a zone of high signal intensity. The cervical stroma consists of an inner subglandular zone of low signal intensity (short arrow) and an outer zone of interme¬diate signal intensity (long arrow). (b) Image shows restriction of diffusion in the subglandular area (arrows). (c) Apparent diffusion coefficient (ADC) map gives a value of 1837 X 10-6 mm2/sec in the subglandular area (empty oval). Stromal ADC was measured in an adjacent area (filled oval). The patient gave birth 34 days later.
High-res (TIF) version
(Right-click and Save As)
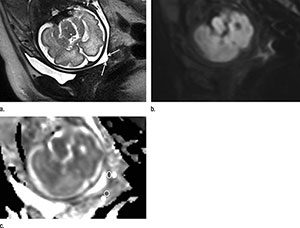
Figure 2. Images in a 28-year-old woman at 30 weeks of gestation with a sonographic cervical length of 8 mm who was referred for evaluation of suspected corpus callosum dysgenesis. (a) MR image shows a short cervix with funneling (arrows). The cervical canal appears as a zone of high signal intensity. (b) Oblique sagittal DW image shows a uniform hypointense subglandular area of the cervix without any restriction of diffusion. (c) Apparent diffusion coefficient (ADC) map gives a value of 2681 X 10-6 mm2/sec in the subglan¬dular area (empty oval). Stromal ADC was measured in an adjacent area (filled oval). The patient gave birth 4 days later.
High-res (TIF) version
(Right-click and Save As)
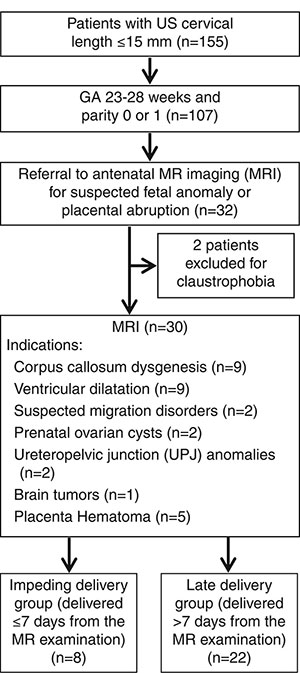
Figure 3. Flowchart of participants in this study. GA = gestational age.
High-res (TIF) version
(Right-click and Save As)
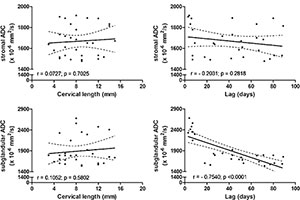
Figure 4. Graphs show correlation between the stromal and subglandular ADC and cervical length and interval between MR imaging and delivery. The r and P values refer to Bravais-Pearson linear correlation applied to evaluate the relationship between different parameters. The best-fit line (solid line) and its 95 percent confidence bands (dashed lines) are plotted on each graph. Lag = interval between MR imaging evaluation and date of delivery.
High-res (TIF) version
(Right-click and Save As)
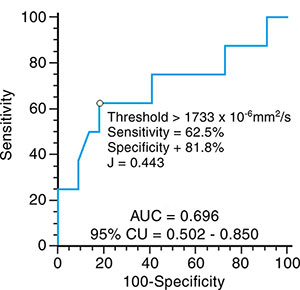
Figure 5. Receiver operating characteristic (ROC) curve analysis of stromal apparent diffusion coefficient (ADC) in patients with a sonographic short cervix between 23 and 28 weeks of gestation. The blue line corre-sponds to the ROC curve obtained with the optimal threshold value (⃝). The optimal threshold value, sensitivity, specificity, Youden index (J), and area under the ROC curve (AUC) and its 95 percent confidence interval are reported. ROC curves of subglandular ADC and ADC difference have been omitted because they are perfect (AUC = 1.000).
High-res (TIF) version
(Right-click and Save As)
